Our Benegration Data Warehouse eliminates the traditional siloed approach to managing a benefits program by effectively aggregating, integrating, and analyzing our clients’ plan data. We collect a variety of health, wellness, and employee demographic data from the members, carriers/vendors, and the employer. This data is integrated into a single platform giving our clients (not the carriers/vendors) control of their own data. Through effective data mining, our solution performs clinical management oversight to identify utilization patterns of the plan’s members, to help employers understand what’s driving their healthcare costs and detect any gaps in care for members.
Our Data Warehouse analyzes that same group-specific data to enable our clients to effectively understand the financial aspects of their plans through state-of-the art claims, utilization, and trend analysis. This enables our clients to prepare budgets and forecasts, analyze alternative funding and plan design strategies, effectively negotiate and manage vendor contracts, and reduce overall benefit costs.
Data Warehouse
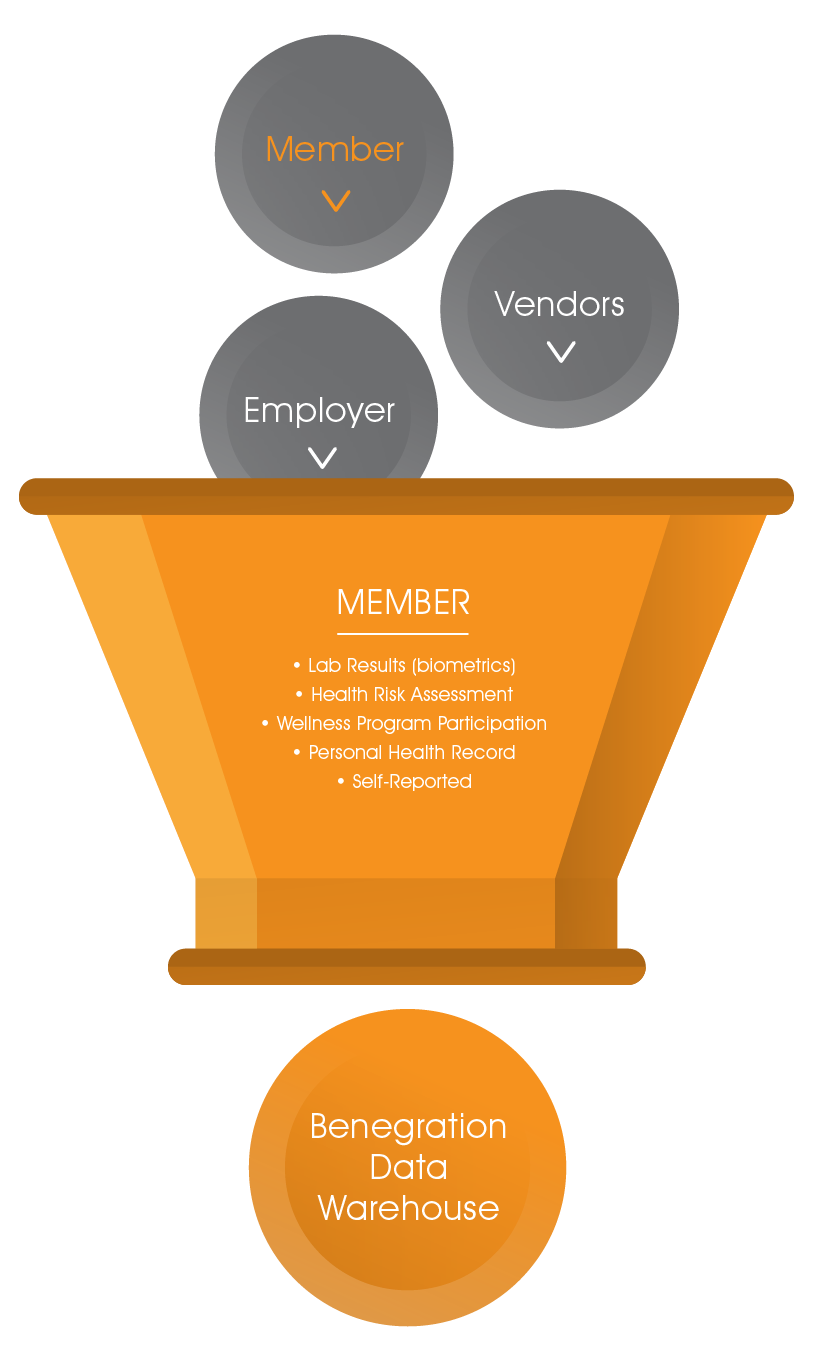
Our proprietary Data Warehouse eliminates the silos by integrating data from three sources:
Members – lab results, health risk assessment, wellness program data, personal health record, and self-reported information
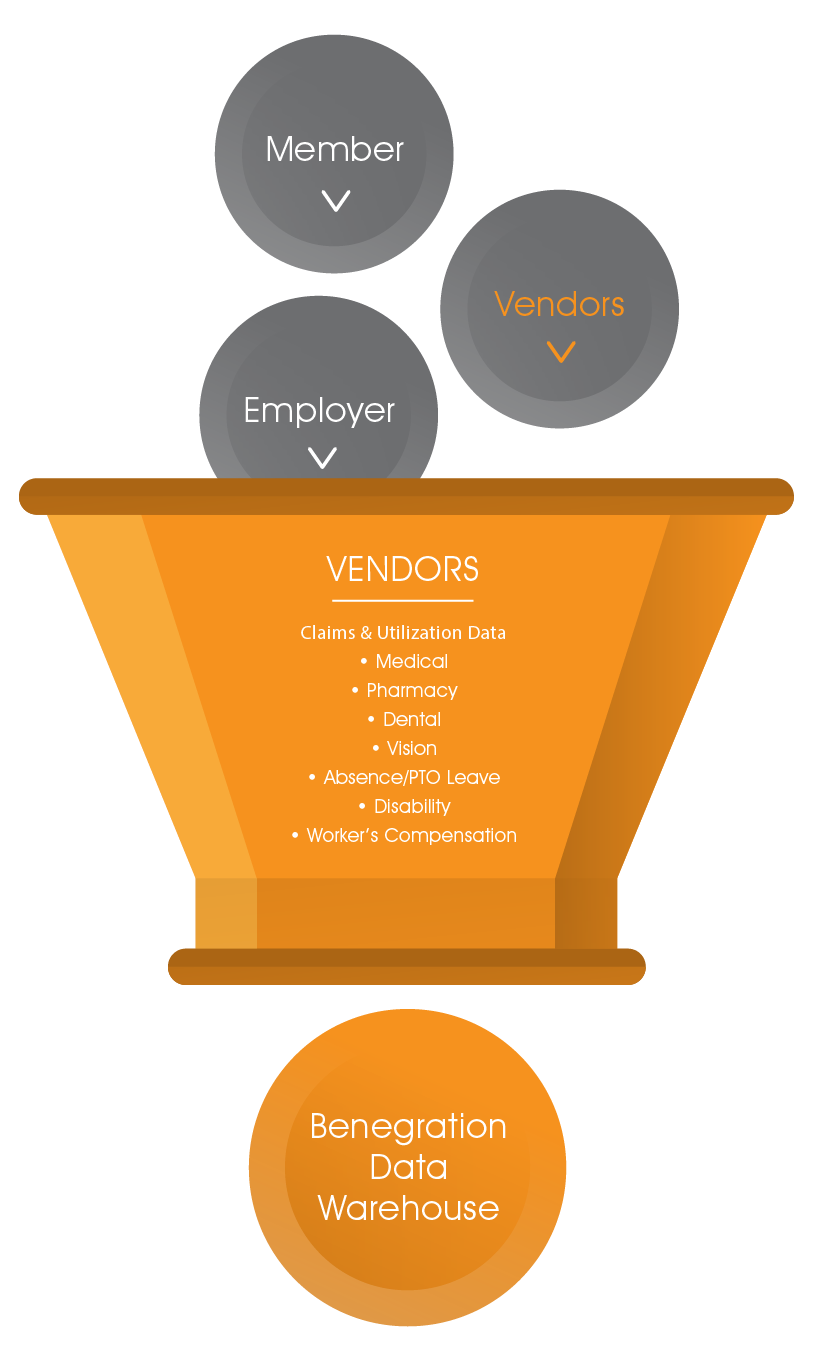
Carriers and Vendors – claims and utilization data for medical, pharmacy, dental, vision, absence/leave/PTO/disability, and workers’ compensation
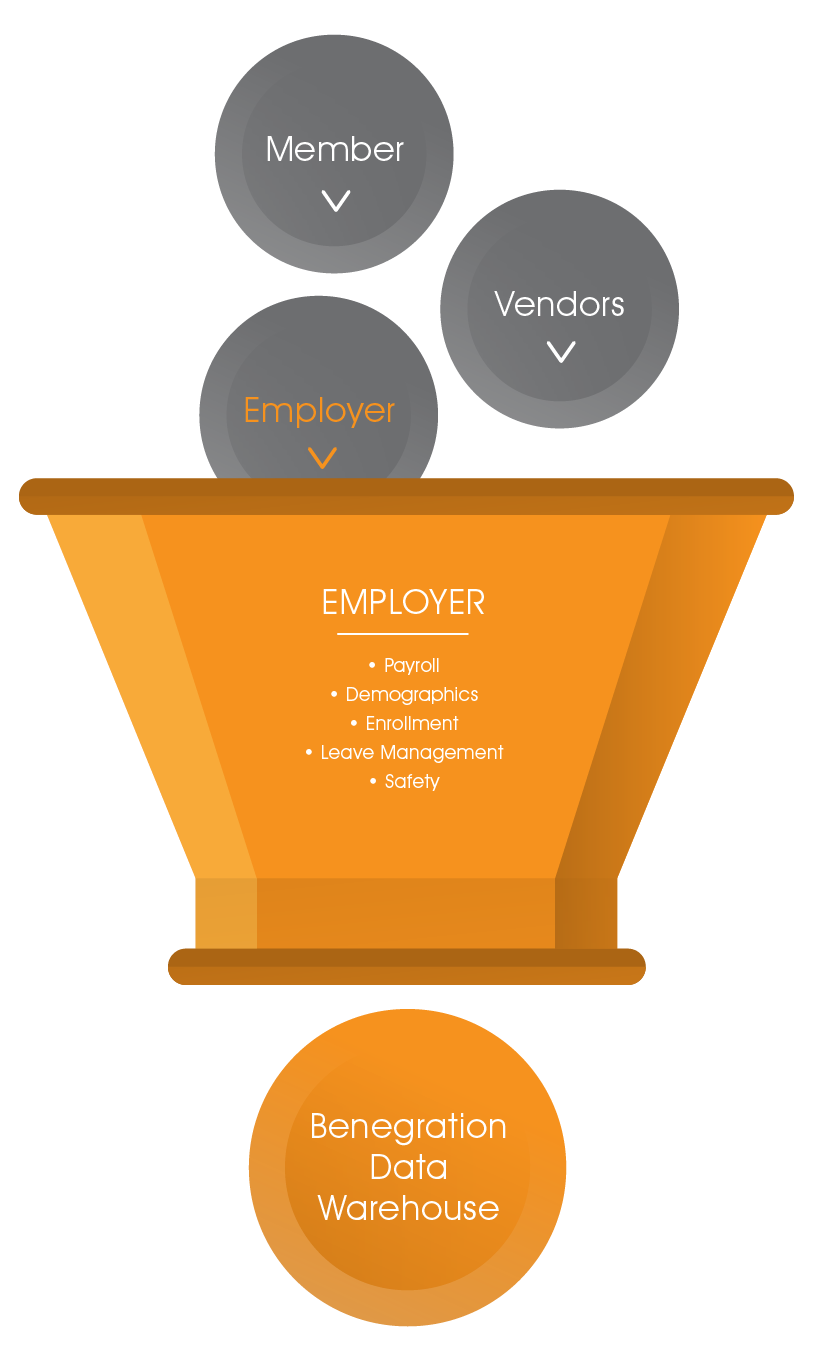
Employer – payroll, demographics, enrollment, leave management, and safety
The pooled data is then integrated and aggregated into a single repository to allow our analysts and consultants to analyze the information. The employer, not the insurance carrier or third-party administrator, controls the data. This model also enables our client to ‘plug and play’ any carrier/vendor (no longer ‘forced’ to bundle several lines of coverage with a carrier in order to receive integrated management and reporting).
Clinical Management & Oversight
Through our data analytics, we are able to provide proactive insight to help clients manage their plans from a clinical, financial, claims administration, and vendor performance perspective using the following approaches:
- Data Mining
- Participant Stratification
- Identification of Cost Drivers (chronic and acute conditions)
- Gaps in Care
- Predictive Modeling
- Clinical Oversight and Intervention
Financial Management & Oversight
Another outcome of our Data Warehouse is the ability to provide our clients with meaningful financial reporting and analysis to help them effectively manage their plans. Our approach includes:
- Baseline Plan Audits
- Routine Performance Monitoring (RPM)
- Financial and Utilization Reporting and Analytics
- Budgets and Funding Analysis
- Financial Forecasts